If you’ve recently had a tooth pulled and you’re wondering whether your healing is going well or something has gone wrong, understanding the difference between a healthy socket vs dry socket is exactly what you need right now. A healthy socket after tooth extraction forms a dark blood clot that protects the underlying bone and nerve, while a dry socket — medically called alveolar osteitis — occurs when that clot is dislodged or fails to form, leaving the bone exposed and causing intense, throbbing pain. The healthy socket vs dry socket distinction is critical because dry socket affects roughly 2–5% of all extractions and up to 30% of lower wisdom tooth removals, and catching it early can save you from days of unnecessary suffering. In this guide, you’ll learn exactly how to identify a healthy healing socket, recognize the warning signs of dry socket, understand why it happens, and know when to call your dentist.
Key Takeaways
- Healthy socket has a dark clot; dry socket looks empty and bony.
- Dry socket pain worsens after day 2–3, unlike normal post-extraction soreness.
- Smoking and straws are the top preventable causes of dry socket.
- Professional medicated dressing provides fast dry socket pain relief.
- See your dentist immediately if pain worsens or bone is visible.
What Is a Healthy Socket After Tooth Extraction?
When a tooth is removed, the empty space left in your jawbone is called the extraction socket. Under normal healing conditions, a blood clot forms within minutes to hours after the procedure. This clot acts as a biological bandage — it covers the exposed bone and nerve tissue, stops bleeding, and creates the foundation for new tissue growth.
A healthy socket typically looks dark red or deep burgundy due to the blood clot. The surrounding gum tissue may appear slightly swollen and pinkish-white around the edges — this is normal granulation tissue forming as part of the healing process. You may notice mild tenderness and swelling in the first 48–72 hours, but the pain should gradually improve with each passing day.
Key characteristics of a healthy healing socket include steady pain reduction over time, no visible bone or white/yellow tissue at the center of the socket, a blood clot that appears dark and intact, and mild swelling that peaks around day two then fades.
What Is Dry Socket? (Alveolar Osteitis Explained)
Dry socket, or alveolar osteitis, is a post-extraction complication where the protective blood clot either dissolves prematurely, gets dislodged, or never fully forms. Without this clot, the jawbone and nerve endings inside the socket become directly exposed to air, food, saliva, and bacteria — resulting in intense, radiating pain that often extends toward the ear, eye, or neck on the same side of the face.
Unlike normal post-extraction soreness that gradually improves, dry socket pain typically worsens after day two or three. It does not respond well to standard over-the-counter pain relievers, which is one of the clearest signals that something is wrong.
Healthy Socket vs Dry Socket: Side-by-Side Comparison
| Feature | Healthy Socket | Dry Socket |
|---|---|---|
| Appearance | Dark blood clot visible | Empty socket, visible bone or pale tissue |
| Pain pattern | Decreasing over 2–3 days | Worsening after day 2–3 |
| Pain intensity | Mild to moderate, manageable | Severe, throbbing, radiating |
| Odor | None or mild | Bad breath / foul taste |
| Onset of concern | No concern | Day 2–5 post-extraction |
| Blood clot present | Yes | No or partially dissolved |
| Response to OTC pain meds | Good | Poor or none |
| Bone visible in socket | No | Often yes |
Healthy Socket Appearance vs Dry Socket Appearance
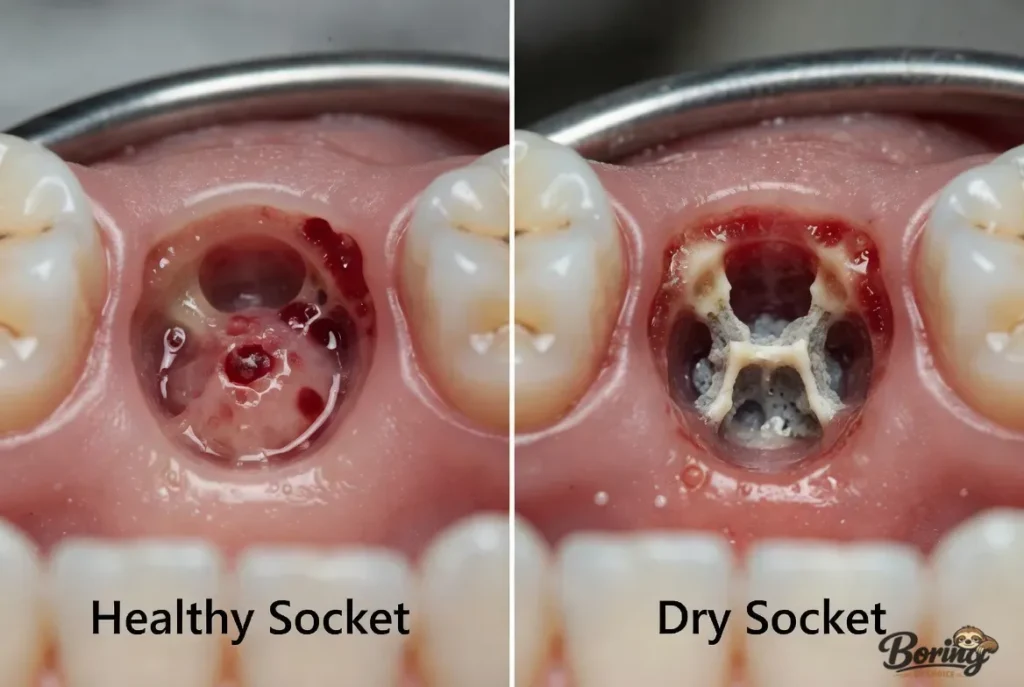
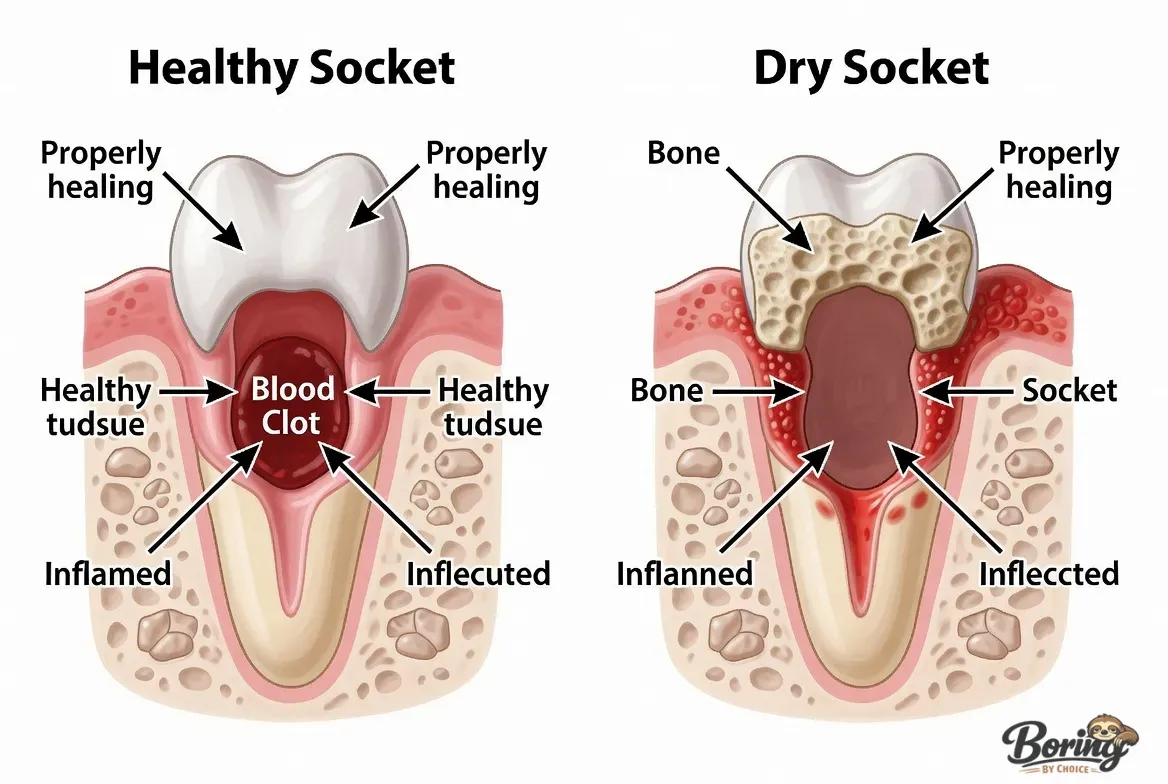
Healthy socket: When you gently look at a healing extraction site (using a mirror and light), you should see a dark clot — almost like a dark maroon or black mass filling the hole. The surrounding gum tissue will be pink, possibly a bit puffy, but it will be covering the edges of the socket normally. Within a week, the clot begins to be replaced by soft granulation tissue, and the socket starts to close.
Dry socket appearance: In contrast, a dry socket looks noticeably empty. You may see a whitish or grayish-yellow hollow area where the clot should be, or in some cases, you can directly see the yellowish-white bone at the base of the socket. The gum tissue around the edges may look inflamed and irritated. If you tilt your head toward a light and the socket looks hollow rather than filled, dry socket is a serious possibility.
Dry Socket Symptoms You Should Not Ignore
Dry socket is one of the most painful dental complications a person can experience. The symptoms usually develop two to four days after extraction and include severe, throbbing pain that radiates from the extraction site toward your ear, temple, eye, or neck; an empty-looking or visibly bony socket; bad taste in your mouth that doesn’t go away with brushing; unpleasant odor from the socket; and swollen lymph nodes around the jaw or neck in more severe cases.
The radiating pain is a hallmark feature. Many patients describe it as a deep, bone-level ache that no amount of ibuprofen or acetaminophen seems to touch. This happens because without the clot, the trigeminal nerve — the major sensory nerve of the face — is directly irritated.
Why Does Dry Socket Happen?
Dry socket occurs when the protective blood clot is lost or impaired. Common causes and risk factors include smoking or using tobacco within 72 hours of extraction (the suction action and chemicals both disrupt clot formation), drinking through a straw during recovery, vigorous rinsing or spitting in the first 24 hours, certain medications like oral contraceptives that can interfere with clotting, a history of dry socket after previous extractions, lower wisdom tooth extractions (which carry significantly higher risk than upper teeth), and poor oral hygiene or active infection at the time of extraction.
Women are statistically more prone to dry socket than men, partly due to estrogen levels affecting clot stability, and partly because oral contraceptive use is a documented risk factor.
How Is Dry Socket Treated?
If you suspect dry socket, the most important step is to contact your dentist or oral surgeon promptly — this is not a condition that resolves on its own without intervention. Treatment is straightforward and brings rapid relief.
Your dentist will gently flush the socket to remove any debris, then pack it with a medicated dressing, often containing eugenol (clove oil) combined with zinc oxide or similar agents. This medicated packing provides immediate pain relief by soothing the exposed nerve tissue. The dressing may need to be changed every one to three days until healing resumes.
In addition to the dressing, your dentist may prescribe antibiotics if there are signs of infection, stronger prescription pain medication for short-term use, and a chlorhexidine rinse to prevent bacterial contamination during healing.
Patients who receive proper dry socket treatment typically experience significant pain relief within 24 hours. Complete healing may still take one to two weeks longer than a normal extraction.
Home Remedies for Dry Socket: What Actually Helps
While professional treatment is necessary for true dry socket, there are supportive measures you can take at home while waiting for your appointment or to complement professional care. Clove oil (eugenol) applied very carefully with a cotton ball can temporarily numb the area — this is the same ingredient used in professional dry socket dressings. Cold compresses applied to the outside of the jaw can help manage swelling and discomfort. Staying well hydrated, eating soft foods, and avoiding any form of suction (straws, smoking) are essential. Over-the-counter pain relievers like ibuprofen can offer modest relief even if they don’t fully control dry socket pain.
Do not attempt to rinse aggressively, probe the socket, or apply any household substances to the wound. Home remedies are supportive only — they cannot replace the medicated dressing your dentist provides.
Healthy Socket Healing Timeline: What to Expect Day by Day
Understanding the normal healing timeline helps you recognize early when something is wrong.
Day 1: Bleeding and clot formation. Some oozing is normal for several hours. Pain is moderate and well-controlled with prescribed or OTC medication.
Day 2–3: Swelling and bruising may peak. Pain should be improving, not worsening. The clot appears darker and more firmly in place.
Day 4–7: Soft tissue begins growing over the clot. Swelling steadily reduces. Pain should be minimal and manageable without strong medication.
Week 2–3: The socket continues filling in from the bottom up with granulation tissue. The opening visibly narrows.
Weeks 4–8: Soft tissue closure is mostly complete. Bone remodeling continues underneath for several months.
Red flag: Any pain that worsens after day three, or that requires stronger medication than you needed on day one, is a warning sign requiring professional evaluation.
When to Call Your Dentist
You should contact your dentist or oral surgeon if your pain is getting worse after the second or third day rather than improving, if you can see exposed bone or an empty socket when you look with a mirror, if you develop a fever above 101°F (38.3°C), if you notice pus or unusual discharge from the site, if the bad taste or odor in your mouth is persistent and worsening, or if over-the-counter pain medications are providing little to no relief.
Do not wait to see if it gets better on its own. Dry socket does not heal without treatment, and delaying care only prolongs your pain.
Preventing Dry Socket: Best Practices After Tooth Extraction
Prevention is always better than cure. Following your dentist’s post-extraction care instructions carefully significantly reduces your risk. For the first 24 hours, avoid rinsing your mouth, spitting forcefully, or drinking through a straw. After 24 hours, gently rinse with warm salt water (one teaspoon of salt in 8 oz of water) after meals. Do not smoke for at least 72 hours — ideally longer. Eat soft, cool foods like yogurt, mashed potatoes, smoothies (no straw), and scrambled eggs. Sleep with your head slightly elevated for the first couple of nights to reduce swelling. Avoid carbonated beverages and alcohol during the initial healing period. Maintain gentle oral hygiene around the site without directly brushing the socket.
If you have a history of dry socket, tell your dentist before the extraction so they can take preventive measures such as applying a clot-stabilizing agent to the socket.
Frequently Asked Questions
How do I know if I have a healthy socket or dry socket? A healthy socket has a visible dark blood clot, improving pain after day two, and no bad odor. A dry socket looks empty or bony, causes severe worsening pain after day two or three, and often has a bad taste or smell.
What does a healthy extraction socket look like? A healthy socket is filled with a dark red or maroon blood clot. The surrounding gum tissue is pinkish and may be slightly swollen, but the socket is not hollow or visibly bony.
How long does a healthy socket take to heal? Soft tissue closure typically occurs within two to three weeks. Complete bone healing underneath takes several months, but most people are comfortable and symptom-free within one to two weeks.
Can dry socket heal on its own without treatment? Dry socket does not resolve quickly on its own. While it will eventually heal without treatment over several weeks, the pain is severe and prolonged. Professional treatment provides immediate relief and prevents complications like infection.
Is it normal for a socket to look white or yellow after extraction? The gum edges around a healthy socket may look slightly whitish or yellowish in the first few days — this can be normal fibrin tissue. However, if the center of the socket (where the clot should be) looks white, hollow, or reveals bone, that is a warning sign for dry socket.
What does dry socket smell like? Dry socket typically produces a foul, unpleasant odor coming from the extraction site. This is caused by bacterial activity in the exposed socket. A persistent bad taste that doesn’t respond to brushing is a common complaint.
How quickly does dry socket treatment work? Most patients experience significant pain relief within 24 hours of receiving a medicated dressing. Some feel improvement within just a few hours of treatment.
Who is most at risk for dry socket? Smokers, oral contraceptive users, people with a history of dry socket, and those undergoing lower wisdom tooth extractions are at the highest risk.
Conclusion
Knowing the difference between a healthy socket vs dry socket gives you the ability to act quickly and confidently after a tooth extraction. A healthy socket heals progressively, with pain improving each day and a visible dark clot protecting the wound. Dry socket, on the other hand, is characterized by worsening pain, an empty or bony-looking socket, and a foul odor — all signs that the protective clot has been lost and professional care is needed without delay. Follow your dentist’s aftercare instructions carefully, avoid smoking and straws, and do not hesitate to call your dental office if something feels wrong. With prompt treatment, dry socket resolves quickly, and your recovery can get back on track.








Leave a Reply